 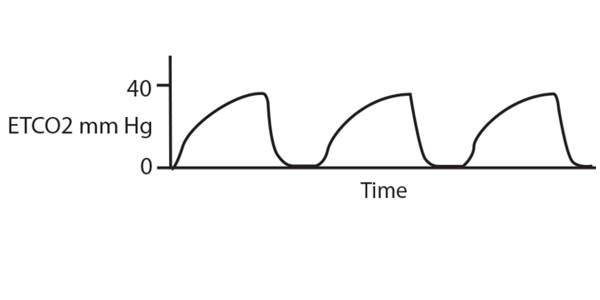
Set up: As the PGY-2s transition to the trauma airway, cardiac and resus role, make sure you have this in each of your bays. If you are working in an emergency department that has capabilities of measuring EtCO2, it can be a very helpful tool to monitor ventilation during procedural sedation! Being the black cloud that I am, this of course has happened to me. In this case, the pulse ox may not desat immediately and it can be helpful to know early when you should stimulate the patient, jaw thrust them or get the BVM ready if the EtCO2 drops to 0. Oftentimes we provide supplemental oxygen for passive oxygenation to prevent desaturations in the case the patient hypoventilates or becomes apneic during procedural sedation. His reasoning is that pulse ox saturations take time to drop, especially if you are providing supplemental oxygen. However, in 2018 ACEP guidelines gave a level B recommendation regarding routine use of capnography during procedural sedation given that literature has not proven that it reduces adverse respiratory events. A sudden increase in EtCO2 greater than 10 from the patient’s baseline can be an early indication of ROSC.ĮtCO2 monitoring during procedural sedation: We use this commonly in the form of nasal cannula with end tidal to monitor for apneic events during procedural sedation. EtCO2 less than 10 suggests inadequate CPR or a low likelihood of survival at the 20 min mark. However if you are giving good quality compressions you can get adequate blood flow to the lungs to produce a measurable EtCO2. Remember that in an arrested patient, lung perfusion and gas exchange at the level of alveoli is not occurring. EtCO2 became a level 1 recommendation by AHA in 2010 for tube confirmation in patients undergoing CPR. However, this should taper after a few breaths.Īlso important to note: right main-stem intubation may still have a normal EtCO2, so get a CXR to confirm tube positioning.ĮtCO2 monitoring during Cardiac Arrest: EtCO2 can be used as a reflection of quality of CPR (optimal depth and rate) and may indicate prognostication for ROSC. Esophageal intubation can initially produce an EtCO2 due to gastric CO2. If the tube is in the right place, you should have EtCO2 with a good waveform on the monitor. Tube Confirmation during Intubation: EtCO2 is the gold standard used to confirm endotracheal tube placement in the trachea and to monitor effective ventilation post intubation. I have included some interesting ones below. There are so many different capnography waveforms, depending on the patient’s physiology and pathology. I nterpreting the waveform: When your patient is connected to end-tidal, you can interpret what you see on the monitor by looking at the various phases. However in patients with lung disease, pathological dead space can increase this gap. 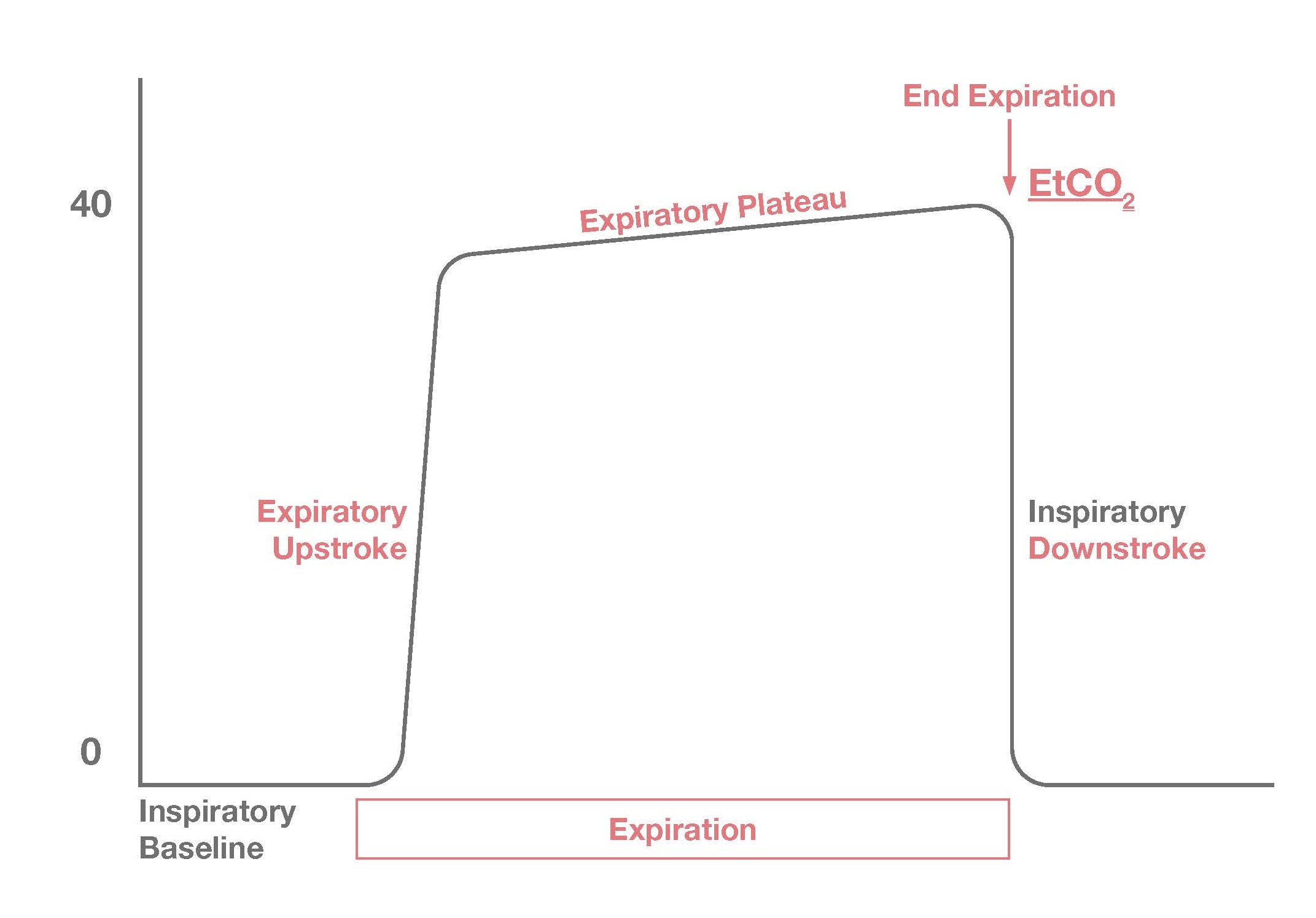
In a healthy patient with healthy lungs the difference between the EtCO2 and PaCO2 is usually less than 10mm. As a result, EtCO2 value is typically lower than PaCO2. The gas from the alveoli during expiration is being diluted with the gas in the dead space (roughly 150cc). This dead space (not very hard-working) does not help clear CO2 since it does not participate in gas exchange. However as we expel air out of our lungs it encounters anatomic dead space (trachea/bronchi). The CO2 pressure in the alveoli should roughly match the arterial CO2 (PaCO2). Remember, blood flows to the alveoli, and boom – gas exchange occurs. Let’s talk about our lovely hard-working functional alveoli – doing their thing and ventilating our bodies. It is affected by ventilation, pulmonary perfusion, and CO2 production. It provides a numeric value of exhaled carbon dioxide. What is EtCO2? It is a measurement of the partial pressure of CO2 in the gas sample at the end of expiration. If equipment for EtCO2 monitoring is available, use it! Role during Procedural Sedation: Monitors for hypo-ventilation and apneic events allowing for early intervention. A sudden increase in EtCO2 greater than 10 from the patient’s baseline can be an early indication of ROSC. If it starts to drop, consider switching compressors or making sure the LUCUS is in the appropriate position. 
0 Comments
Leave a Reply. |
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |

 RSS Feed
RSS Feed
